“If our skin is grass and the layer underneath is the dirt, I’m missing the roots of the grass that hold the skin down so that the grass doesn’t come off when people walk on it. I’m missing the thing that holds the skin together. With any minor trauma, my skin can just peel right off.”
Exciting News: VYJUVEK is now approved for use from birth, can be applied by a caregiver or patient at-home, has an increased weekly volume, & has the flexibility of being removed at your next dressing change.
What Is Dystrophic Epidermolysis Bullosa (DEB)
DEB is a genetic condition that causes blisters and scarring of the skin
DEB wounds can range from very small to large, take a long time to heal or not heal at all, and are prone to reopen after healing.
DEB is caused by changes in the gene that gives the body instructions to make a protein called type 7 collagen
- Proteins are the building blocks of your body, each with a specific job
- The job of type 7 collagen is to hold the inner and outer layers of the skin together
- Without type 7 collagen, the inner and outer layers of your skin can easily separate with any type of friction, making your skin fragile
- Weakened skin leads to blisters, wounds, and scars
There are 2 types of DEB:
- Dominant DEB (DDEB)
- Recessive DEB (RDEB)
What Causes DEB?
DEB is caused by changes in the gene that gives the body instructions to make type 7 collagen.
All DEB wounds should be taken seriously. It’s possible for any DEB wound to develop complications, including a certain type of aggressive skin cancer called squamous cell carcinoma (SCC).




Skin with
type 7
collagen
Skin with
DDEB
Skin with
RDEB
How genes carry DEB
Genes carry instructions that tell the body how to build specific proteins. When there is a change in these instructions, the body cannot make the protein correctly, which leads to DEB.

Gene


Functional
proteins

Gene


Non-functional
proteins
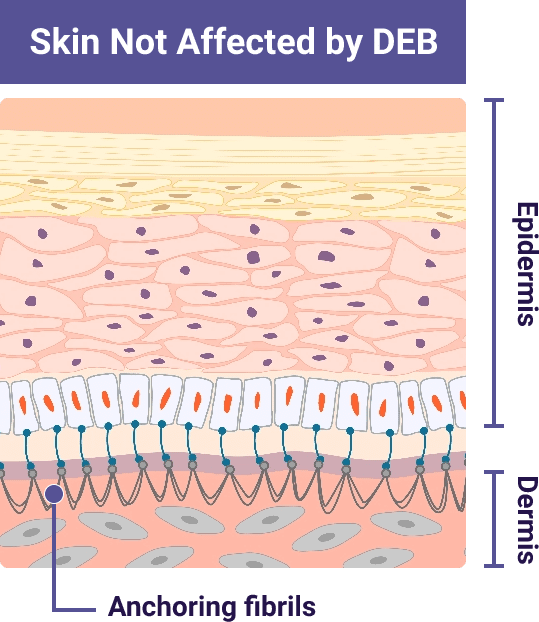
The COL7A1 gene carries instructions to make type 7 collagen, which is a protein
Type 7 collagen is the main component of anchoring fibrils. Anchoring fibrils help bind the inner skin layer (dermis) and outer skin layer (epidermis) together
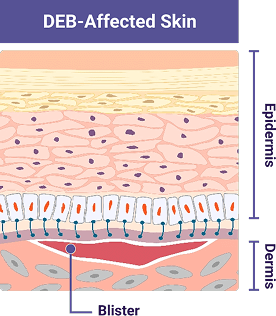
In people with DEB, the change in the COL7A1 gene means the body cannot create enough working type 7 collagen protein
This leads to a lack of or reduction of working anchoring fibrils. Without working anchoring fibrils, the skin layers can easily separate due to friction
- Illustrations adapted from De Rosa L., Latella MC, Secone Seconetti A, et al. Cold Spring Harb Perspect Biol. 2020.
There are 2 types of DEB
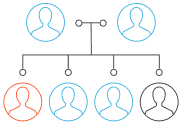
Recessive dystrophic epidermolysis bullosa (RDEB)
Neither parent has RDEB but both are carriers of the recessive gene. Each child has a 25% chance of inheriting the recessive gene from both parents and being born with RDEB.
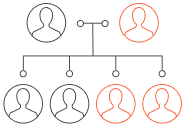
Dominant dystrophic epidermolysis bullosa (DDEB)
At least one parent has DDEB. Each child has a 50% chance of inheriting the dominant gene and having DDEB.
-

Unaffected person
-

Gene carrier
-

Person with DEB
In DEB (DDEB and RDEB), your body does not make enough type 7 collagen.
No matter the severity of your DEB, it’s important to restore your skin’s ability to make type 7 collagen for wound healing.
A Family Finds Answers
It’s important to accurately confirm DEB
DEB symptoms can resemble other epidermolysis bullosa (EB) types, such as EB simplex, and even other skin conditions. This means diagnosis based on symptoms alone can be unreliable.
Tests to confirm DEB include:
Skin biopsy can help show EB type, but it may be incomplete or inaccurate and may not be able to distinguish dominant DEB (DDEB) from recessive DEB (RDEB).
Genetic testing uses a sample of blood, saliva, or a cheek swab and can accurately identify DEB, as well as determine:
- Gene change
- Whether the condition is DDEB or RDEB
VYJUVEK is a topical gel used to treat wounds in adult and pediatric patients (from birth) with dystrophic epidermolysis bullosa (DEB).
VYJUVEK gel should be applied by a healthcare professional, patient, or caregiver.
After treatment, patients and caregivers should be careful not to touch treated wounds and dressings until the next bandage change. If accidentally exposed to the VYJUVEK gel, clean the affected area.
Wash hands and wear protective gloves when changing wound dressings. Disinfect bandages from the first dressing change with a virucidal agent and dispose of the disinfected bandages in a separate sealed plastic bag in household waste. Dispose of the subsequent used dressings in a sealed plastic bag in household waste.
The most common adverse reactions (>5%) were itching, chills, redness, rash, cough, and runny nose. These are not all the possible side effects with VYJUVEK. Call your healthcare provider for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088 or to the Sponsor at 1-844-557-9782.
Please see Important Safety Information above and click here for full Prescribing Information.
VYJUVEK is a topical gel used to treat wounds in adult and pediatric patients (from birth) with dystrophic epidermolysis bullosa (DEB).
VYJUVEK gel should be applied by a healthcare professional, patient, or caregiver.
After treatment, patients and caregivers should be careful not to touch treated wounds and dressings until the next bandage change. If accidentally exposed to the VYJUVEK gel, clean the affected area.
Wash hands and wear protective gloves when changing wound dressings. Disinfect bandages from the first dressing change with a virucidal agent and dispose of the disinfected bandages in a separate sealed plastic bag in household waste. Dispose of the subsequent used dressings in a sealed plastic bag in household waste.
The most common adverse reactions (>5%) were itching, chills, redness, rash, cough, and runny nose. These are not all the possible side effects with VYJUVEK. Call your healthcare provider for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088 or to the Sponsor at 1-844-557-9782.
Please see Important Safety Information above and click here for full Prescribing Information.

